Where HOPE grows, miracles blossom…
– Elna Rae
The Umbrella

6 months ago today I looked upon your beautiful face for the very last time. How have I lived half a year already without you? There’ve been so many “firsts” in the past 6 months – the world kept turning, even when mine came to a sudden halt. I wanted to fall asleep and never wake up, but with each sunrise came a new day. I wanted to believe it was all a bad dream, but with each new day came the harsh realization that you were really gone. I remember, shortly after you left, someone said that losing a child grows harder with time… and I remember thinking it couldn’t possibly be so, because if it got any harder, surely I would never survive. 6 months later and I think it may be true. While the initial shock has subsided, the deep void you’ve left behind is only widening. I miss you fiercely sweet girl… I miss your laugh, your touch, your smell… I miss every ounce of who you were, and I’d give anything to have you here with me again.
Much has changed in my life since Emerson passed. For starters, I’ve stepped away from social media, at least for the time being – for mental health purposes, I needed a break. I’ve also gone back to school full-time to pursue a BS in nursing. I’m taking required science pre-reqs now and will apply to a one-year, accelerated program in the fall. It’s a natural fit, as I provided nursing care to Emerson for nearly 13 years. I only need my license, now, to provide that same care to others. In all, it feels like a constructive way to channel my grief and to honor Emerson. I’ve always believed that good things will come from her life, but only because I/we consciously choose them to. As such, I’m choosing to take what she taught me and use it to help others. It feels right, and the process of getting there has been a healthy distraction and good therapy for me. On a sad note, Jim and I have ended our marriage. It started before Emerson’s death but finalized afterwards and had nothing to do with her passing. We remain committed to the boys and I wish him nothing but continued success and wellbeing in the future. And to top it all off, I’m in the middle of a move that is weighing heavily on me, both physically and emotionally. It’s proving very difficult to leave the home I shared with Emerson and to wake up in a place where she never existed. My head knows, beyond a shadow of a doubt, that she is with me, but my heart aches for memories of her in this space.
It’s hard to not feel like I’ve been caught in a tornado for the past 6 months… make that a 13- year storm leading up to a 6-month hurricane with sustained winds. That said, the strangest thing happened shortly after Emerson passed – I received a message that a UPS package was delivering, 2nd day air, to an address we lived at 3 years ago. Unaware of what it could be, I promptly logged into my UPS account and redirected the package to our new address. Several days later it arrived and I opened it – an umbrella. Nothing fancy, just a black umbrella. No special packaging, no note, no gift receipt… only the box to indicate it had been shipped from the manufacturer. It was clearly addressed to me, but I had definitely not ordered it. The mystery of the umbrella sat with me for months. Baffled by who had sent it, I was thankful to have it. Then a song came on the radio and I listened… then I listened again… it’s a popular song, but I’d never really listened to the words until that day:
“When it rains it pours, but you didn’t even notice
It ain’t rainin’ anymore, it’s hard to breathe when all you know is
The struggle of staying above, the rising water line
Well the sky is finally open, the rain & wind stopped blowin’
But you’re stuck out in the same old storm again
You hold tight to your umbrella, well darlin’ I’m just tryin’ to tell ya
That there’s always been a rainbow hangin’ over your head
Oh tie up your bow, take off your coat, and take a look around
Everything is alright now
Let go of your umbrella, ‘cause darlin’ I’m just tryin’ to tell ya
That there’s always been a rainbow hangin’ over your head”
I still have no idea who sent me that umbrella, perhaps it was a gift from the universe. To whomever did: thank you, but I’m going to try to let go now… I will never, ever get over Emerson’s death and I will have “not okay” days for the rest of my life, I know that. I also know, though, that the sun is shining upon her every day now. She has weathered her storm and found her peace. We are done fighting. She is okay, now I need to be too.
The day before Mother’s Day, in a random pile of papers in the garage, I came across a heart Emerson painted that read: “Happy Mother’s Day! Thank you for taking care of me. I love and miss you. Love, Eme” I have no idea when she made that, (or how it got into a random pile of papers in the garage), or why she would have said she missed me – we were always together! Maybe it was meant for me to find that day, the day before my first Mother’s Day without her. I will choose to believe it was and will cherish it always as a special gift from Heaven on that day.
Six months without you sweet girl – it feels like a lifetime and a blink of an eye, all at the same time. I’m not sure how I survived, but by the grace of God I am still breathing – I fall asleep every night to pictures of your beautiful face and wake every morning to the same. The storm has passed and everything is going to be alright; you are safe and I will survive, on my own – some way, some how. You were a shining example of all that is good in this world. Your beautiful spirit taught me strength in the face of adversity. You taught me to never stop fighting for a better tomorrow, and to never stop searching for rainbows and unicorns; we will find them if only we believe. Because of you, brave girl, I believe.
Celebration of Life
We hope you can join us this Saturday, 1/18, to celebrate the life of one remarkable little girl… her time on this earth was brief, but her impact enduring.
Celebration of Life
Emerson N. White
9/12/06 – 11/15/19
Date: Saturday, January 18, 2020
Location: Denver Botanic Gardens, Marnie’s Pavilion
https://www.botanicgardens.org/
Time: 1-5pm
It is an open house style event, there will be no formal service. Please feel free to come and go as you’re able to between 1-5pm.
Parking at the Botanic Gardens is free as space permits. There are ample spots and, given as January is off-season, they shouldn’t fill up.
All guests will receive free admission to the Gardens for the day. Once parked, please enter through the Visitor’s Center – tell them you’re there for Emerson’s Celebration of Life and they will let you through. Once in the Gardens, signs will mark the path to the event location. It is only a short walk from the entrance.
In honor of Emerson, we ask that you wear pink (if you have any pink in your closet this time of year) and, if you have one, we ask that you come with a story to privately share – I’m building a memory book and would love your input. Cards will be available to record your memory on.
We look forward to seeing you Saturday…
Christmas 2019
Dearest Emerson,
What I wouldn’t give to turn back time… if only I had known what God had planned, I would have held you tight & never let go. I would have made time for extra snuggles, one more story… I wouldn’t have asked you to wait… we would have watched TV together, side by side, all day long… baked cookies & pumpkin bread… If only I had known…
Today was Christmas. The tree looked oddly bare without all your gifts underneath it, and the house was eerily quiet without your boundless anticipation and excitement. I went to church last night in hopes of feeling closer to you, instead the hymns brought tears and sadness beyond comprehension. I promised that I would miss you, that promise I have kept. I also promised that I’d be okay, I’m working on that one my sweet girl.
Six weeks without you feels like a lifetime. It’s hard to understand how someone so full of life can one day simply cease to exist. It doesn’t seem possible, yet my brain knows it happened. Still my heart tries to hide from the truth. I know you would want us to be happy, though, especially today. You loved Christmas, you prepared for this day for months.
In your honor, precious angel, we celebrated today. We laughed and shared memories of Christmases past with you. We looked through photos and shed a few tears, but mostly we smiled. We were so blessed to have you in our lives… we are all better because of you – more patient, more accepting, more loving. Your life was the greatest gift we’ve ever received.
I hope your day was filled with endless Playmobil Hospital sets, L.O.L. Surprise! Dolls, American Girl accessories, and so much more! I can only believe that the celebration in Heaven on this, the birth date of Jesus Christ, was far grander than anything my mind can dare to imagine.
Dearest Emerson, you are so loved & so missed. Until I am blessed to hold you again…
Merry Christmas to all!
We hope you can join us for a Celebration of Emerson’s life, all are welcome.
Date: Saturday, January 18, 2020
Location: Denver Botanic Gardens, Marnie’s Pavilion
1007 York St, Denver CO 80206
Time: 1PM – 5PM
It will be an open house event, there will be no formal service. Please feel free to come and go as you’re able to within that timeframe. All guests will have complimentary access to the Denver Botanic Gardens for the day – there are indoor exhibits, but also outdoor spaces to explore, weather permitting. We ask that you please wear pink (if you have any clothing that color) in Emerson’s honor.
In lieu of flowers, donations can be made in Emerson’s name to: The University of Nebraska Foundation Transplant Fund. More details on how and where to direct those funds will follow.
If you know you’ll be attending and could kindly drop a reply indicating as such, I’d greatly appreciate it. It’s not at all necessary; RSVP is not required. It would be helpful, though, for planning purposes, to have a general idea of how many to expect.
Thank you.
Christmas through the years…





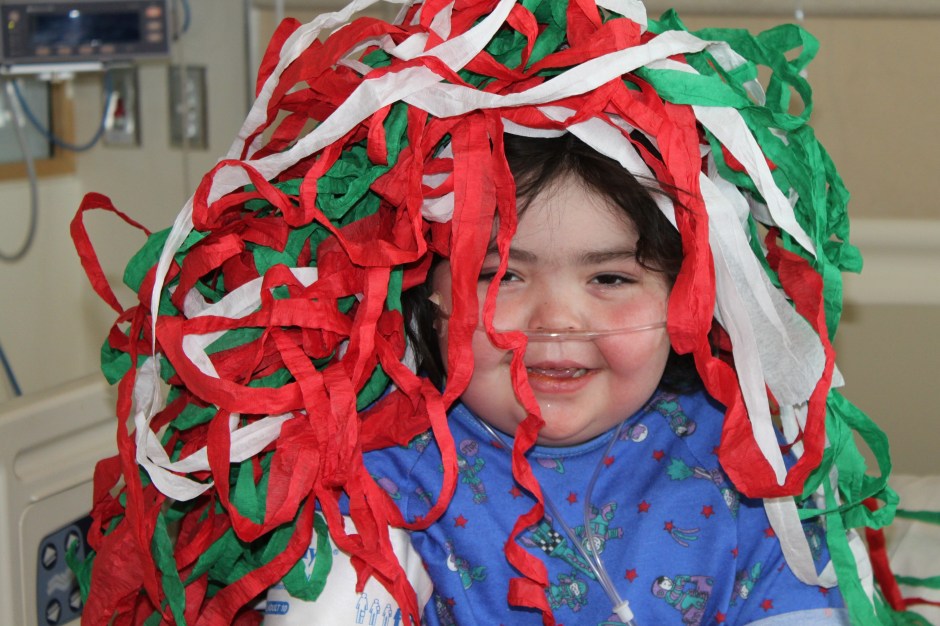
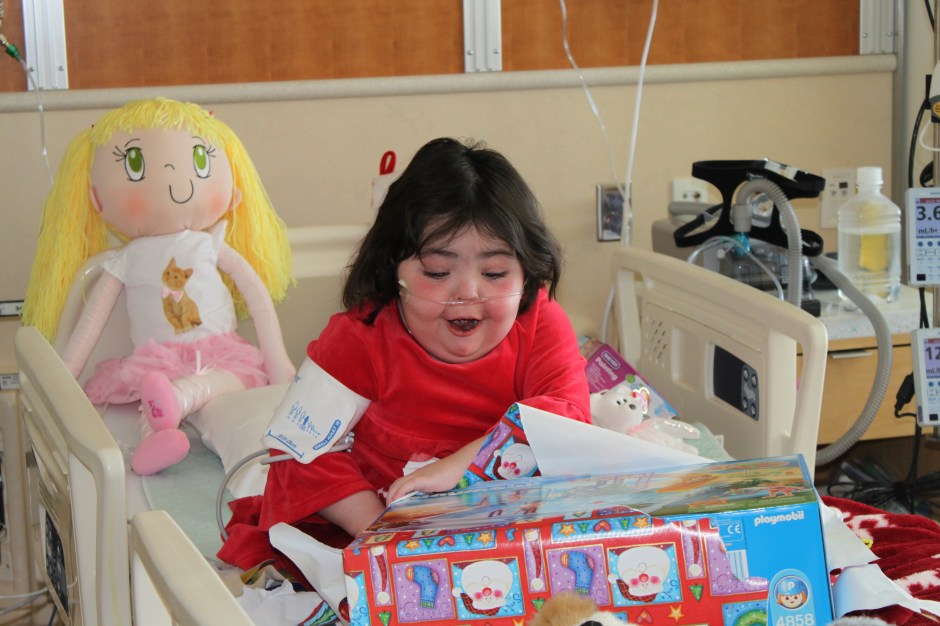











Forever in Our Hearts
It’s been 1 week & I’m still breathing… one day, one hour, one minute at a time.
I’m overwhelmed by the beautiful messages from each of you, they remind me how much Emerson was loved and how much her life had impact & meaning. Thank you.
Eme proved that it is not the years in your life, but the life in your years that matter most… She packed enough love, joy, & inspiration in 13 short years to span a full lifetime. Her days here may have been short, but they were rich & oh so blessed. It was an honor to be her mother & to walk beside her on this journey.
I want to give everyone a brief explanation as to what happened, as so many have asked:
Emerson was doing really well – she had a great Halloween & even weathered a (very) cold night to walk door to door, collecting as much candy as she possibly could. She loved Halloween! Immediately after the costume came off, her focus quickly shifted to her Elf on the Shelf (Candy) who would be arriving on Thanksgiving Day &, of course, Christmas. On Sunday night, 11/10, we sat in bed forever as she scrolled through an endless list of things she’d found on Amazon… each one she “had to have” for Christmas. She was in great spirits. I went to sleep that evening completely oblivious to & unprepared for what the next 5 days would bring…
Emerson awoke Monday morning with a fever. I took her to the local hospital Monday afternoon where they started IV antibiotics, stabilized her, and life flight transferred her to Omaha. She arrived in Omaha early Tuesday morning and passed on Friday. Emerson was in septic shock; blood cultures were positive for both klebsiella and e-coli. Eme deteriorated very quickly upon arrival in Omaha. The many details beyond that are still too raw and painful to recount. Her dad and brothers flew in Wednesday to be with her… heartbroken, we all had time for personal & private good-byes. Her passing was peaceful, she went very quickly and without pain.
The support we received from current & former staff at Nebraska Medicine was incredible – so touching & heartfelt… former PICU nurses came in from home & other jobs, everyone from the transplant team was present… The compassion and empathy from so many helped to ease an impossible situation. There were so many tears, each one reminded me that her life had reach. Every memory reminded me that her battles were not fought in vain.
As I sit here today, 7 days later, I’m not sure I’ve completely allowed myself to accept the reality of what happened. I’m still expecting her to turn the corner or call my name… the silence is deafening. I’ve had many distractions at home from people checking in on me and from the boys who are here until after Thanksgiving break. The distractions have kept my mind busy and helped to protect my heart from the pain. It will take a long time to work through this and I’m not sure I’ve even begun. I lost my best friend 7 days ago… She relied on me & I vowed to protect her always, 7 days ago today I could not.
We are planning a Celebration of Life for Emerson on Saturday, January 18, 2020 at the Denver Botanic Gardens. All are welcome. More details to follow…
Thank you for being a part of Emerson’s journey & for making a place for her in your heart. Your prayers lifted us through the darkest of times & multiplied our celebrations. May the footprints she leaves behind forever imprint themselves upon you. May the lessons she taught carry us all through this life. God bless.
Happy Spring!
2019 started a little rough with a lengthy admission in Omaha, but we’re home now – adjusting to a new med routine and increased level of cares. All in all, Emerson is well, although tired. Managing pain and hydration have been challenging, but thanks to the great team in Omaha who trust me to care for her and who work so well with us from afar, Eme is able to stay at home… with her best friend Bella… & all is well in her world 🙂
While we’re thankful to be back in Colorado, though, our thoughts and prayers are with those affected by the terrible flooding in Nebraska. The pictures are simply heartbreaking; the scope of devastation, incomprehensible. I pray that our friends are safe and that the long road to recovery can soon begin. Love to you all!
Overdue Update
I’m not on Facebook often, but I was recently informed of update requests on Eme’s page and signed in to look. To be honest, it put a pit in my stomach as it’s never my intention to keep you in the dark. It seems trite to say I’m very busy (aren’t we all?), but it’s true. More than that, though, are the lingering after effects of this journey for me. Call it PTSD perhaps. I know other moms who fought alongside me for the lives of their children – similar yet unique journeys, each with their own challenges, blessings, and outcomes – and we all deal with it in our own ways. For me the memories are mostly too difficult to recall, and I do my best to suppress them. After being thrust into the spotlight for years, I crave peace and anonymity.
I’ve always said this happened to Emerson and to our family for a reason, and I’ve always believed something positive will come from it – not by happenstance, but because I decide to create positive change. I still believe that with all my heart, but I’ve had to let it go for now. The pressure it created was crushing – What will it be? What positive change can I create that fits the enormity of our journey?… it will have to be big, the price we paid is huge. And how on earth am I going to find the time and energy right now to accomplish it? I have faith it will come full circle in time, but for now I’m accepting that perhaps it just happened. No rhyme or reason or greater good, it just happened. Indeed our journey isn’t over yet; I’m still in the dugout fighting. And maybe for now, that’s enough. Maybe for now, caring for Emerson is all I have to do.
That said, I appreciate those who’ve followed alongside us through the years and I acknowledge the incomparable healing power of all your prayers. It’s not my intention to only update when Eme is in the hospital, but that, of course, is when I have time to do so. Our lives are chaotic and constantly changing – it’s all good, but crazy! Never a dull moment in the White household!
Emerson is (knock on wood) doing pretty well. We’ve been extra careful this winter & have all, so far, been spared this season’s nasty flu. And a new central line last fall, along with a new line protocol, has kept her infection free and out of the hospital. We are seeing an increasing decline in her kidney function, however, and weekly labs are concerning for the health of that transplanted organ. The dietician is adjusting Eme’s TPN formula weekly to accommodate for the kidneys’ declining ability to filter essential electrolytes from her bloodstream. There’s no doubt it’s a concerning development. We’re planning a trip back to Omaha soon to meet with nephrology and her transplant team.
Clinically, Eme has slowed down… despite a “healthy” winter, she doesn’t have the energy to do much these days. She’s sleeping more and tiring out quickly; we rarely leave home without her wheelchair anymore.
Educationally, we made the decision to home-school Emerson this year. Adding one more thing to my plate everyday has been a challenge, but we felt it best to control her exposure to germs in the winter months and also to provide her more targeted learning opportunities. As she progressed in grades at school, the classroom material simply became too difficult for her. Eme, as a likely result of 2 cardiac codes, has a very hard time grasping basic educational concepts. At age 11, she’s been working on writing her name, “EME”, for 6+ years with continued inconsistency. At home, we’re working our way through identifying letters of the alphabet and learning their sounds. It’s a tedious process! She’s so wise and savvy in so many ways, but educational concepts are a significant struggle.
Thank you, as always, for your concern and for your prayers… they are felt.
Happy spring to all!
Shhhhhh…..
Eme is discharging in about an hour. Don’t cheer too loudly, we don’t want to jinx it 😉
The Umbrella Effect
We are never getting out of here.
Emerson continues on lots of IV support. Twice they’ve tried to turn off her PICU drip – the first time she lasted about 15 minutes, the second time hours, but not long. She’s back on vasopressin this morning to control excessive urine output and resulting electrolyte imbalances. Add to that increased ostomy output from her transplanted bowel, and managing Eme’s fluid balance continues to be a very big challenge. Basically her transplanted organs (kidneys and bowel) are in abundant overdrive, wasting excessive fluid & critical electrolytes.
To illustrate the degree to which Emerson is struggling: average & acceptable urine output for her is roughly 50-70 mls/hour; her kidneys are excreting 500-700 (even up to 1,200) mls/hour. Her bowel output is over triple what it should be and significantly increased over her “norm”.
The infection that brought Emerson in is a distant memory. The resulting organ fall-out from the infection, though, is proving to be the hurdle we can’t jump.
Many really great doctors are involved and no one knows what to do. I just had a lengthy conversation with a senior endocrinologist here and he stated the rather obvious – Emerson is extremely complicated. He said they’ve been discussing her for a month, and she is the most involved and puzzling case he’s seen (and he paused)… in a very long time, if not ever.
It’s August 1st and this week marks 4 weeks inpatient. Bradley embarks on a new academic/athletic adventure in 14 days and Collin is off to college (yikes!) in 18. We have to get home. We had a few weeks, but time is up. We desperately need to get home.
In a nutshell, we’re never getting out of here. It’s the umbrella effect – you plan for rain, it doesn’t come; you don’t plan for it and it does. So, I’m shaking things up a bit. Maybe planning to be here forever means we’ll actually get out. I don’t know… thinking she’s going to discharge “next week” hasn’t worked. Maybe this will. Ugh.
Gratitude
My thoughts & feelings from yesterday persist, but today I’m choosing to focus on a positive. It’s nearly unheard of that a hospitalization doesn’t result in a life flight transfer to Omaha these days, and this time it did not. This hospital has taken the time to carefully consider all of Emerson’s past medical history as well as her current medical complications. They’ve talked extensively to transplant surgeons and the PICU team in Omaha, even communicating events as they happened in the middle of the night.
All in all, there have been a lot of positives in the past three weeks and, moving forward, I’m choosing to focus on at least one a day for the remainder of this admission. Mind you, it won’t magically erase my exhaustion or frustration; but that’s okay. Those feelings are real and justified. Sitting in a PICU with your daughter as she struggles to recover from septic shock is far from invigorating or fun.
Today I am very thankful for the psych team. It began as a consult to address psychosis coming off the vent, then blossomed into many lengthy discussions about Emerson’s mental status at baseline. She’s struggled for many years with violent behavioral outbursts as well as extreme perseveration. It can be difficult to believe just meeting Eme – she is very sweet, quiet, and well-mannered much of the time. When she launches into an outburst, though, a switch flips and that sweet little girl is nearly unrecognizable.
For years it was attributed to her spending too much time in a hospital & becoming accustomed to getting whatever she wanted whenever she wanted it. I’ve been given much parenting advice over the years – walk away from it, don’t give in, detach, yada yada… News flash – I have 2 older boys and this is not my first parenting rodeo; I know how to manage a temper tantrum! What’s more, I have very deliberately not treated Emerson differently when she’s sick. I have the same expectations for her behavior when she’s sitting in a PICU as I do for her when she’s sitting at home.
Mental health is one component of Emerson’s medical picture that has been largely unaddressed. Omaha is not a pediatric hospital and there is no pediatric psych team to consult when we’re there. That’s not to say anyone dismisses it, just that the resources haven’t been available.
The biggest blessing from the psych team this week? They discussed Emerson’s case at length, reviewed all her medical history, and concluded with certainty that her outbursts and perseveration are biologically driven (i.e., they’re not a result of past circumstances or parenting style). Can I get a Hallelujah?! Thank you. It’s not me. I always knew and now it’s medically documented for everyone else to know too! They think it may have happened in one of her cardiac codes, or it may simply be part of her underlying condition. The “why”, though, is less important than the “what” do we do about it.
They eliminated one med, replaced it with a different one, and are starting another new med tomorrow. They’re watching her closely and increasing doses as she tolerates it. The goal is to calm her, but not sedate her. We may not have time to reach the perfect cocktail of meds at the perfect doses for Eme this admission, but I’m so thankful for a team of doctors that is addressing this seriously, and I’m hopeful we’ll, at very least, be in a better spot when we leave. They’re reaching out to psych doctors in Omaha now to find us ongoing support for after discharge. All good and a definite something to be thankful for today!
I had a lengthy discussion with a PICU doctor this afternoon to lay out the plan for Emerson’s drug, fluid, and electrolyte weans. If all goes as planned, she should be buttoned back up and ready to discharge sometime next week. I’m not holding my breath, but I am certainly crossing my fingers. It can’t come soon enough.
Finally, my heartfelt appreciation for sharing your purposeful activities yesterday – I can’t tell you how much fun they were to read! I’m so touched that we’re able to impact others in such a meaningful way. It helps me to see the positive in this crazy journey we are on. Your homework now is to think of one specific thing you are thankful for today…
And one last positive from my day – I stepped outside this afternoon for the first time in three weeks! And with the help of two nurses, a giant IV pole, a big wheelchair, and a travel monitor… Eme came too 🙂
Another New Week
The road to recovery has been bumpy. Twice Emerson spiked a fever and twice broad-spectrum antibiotics were restarted. We continue to struggle with electrolyte imbalances, including low potassium & phosphorus and shifting sodium levels. And an episode of dangerously low blood pressure one night required rescue measures to correct – a lot of nurses drawing up and pushing 60 mL syringes of normal saline through Eme’s central line as quickly as humanly possible.
With a new week comes a new team. It’s a mixed bag – good to have new eyes, but frustrating at the same time. We are not in Omaha &, while our experience here has been good, this is where it gets tough – people don’t know Emerson and the learning curve is steep. It took years of proving the same things over and over again for everyone in Omaha to accept that which they can’t explain… I don’t have the patience to repeat that process here.
In general, I’m tired of not talking. Every morning residents, fellows, and students gather. They read through a list of Eme’s systems, discuss events (at least those that were recorded), hash through her med schedule, postulate the ‘whys’, and propose a plan. Meanwhile I hang my head and listen. Events are incomplete and the ‘whys’ have already been disproven. The plan, usually some version of what ‘should’ work, won’t work. This is a teaching hospital, though, and this is how it is. Every morning the group gathers – they talk; I listen.
Mostly, though, I’m tired of talking. Individually different doctors stop in throughout the day – I’m tired of reminding everyone about what happened last week. I’m tired of trying to convince them that Emerson doesn’t do it this way or that. I’ve been advocating for nearly 3 weeks and I’m tired. There’s no end in sight this morning and I desperately want to go home.
At the end of the day I think the novelty of Emerson has worn off. This team began determined to figure her out… to find a new way of managing her through a crisis… to report back to Omaha with some profound discovery. Slowly, though, one by one, specialists have dropped off and interest has waned. New patients have arrived and new challenges have ensued.
Mind you, they are in contact with Omaha and they have in no way given up, but the vigor with which this team is discussing new and creative thoughts has stalled. Instead we are left with – this ‘should’ work, let’s just keep doing it; speed it up, slow it down, stay the course.
Okay… but it’s not working. With a grand total of 8 organs transplanted over a 10-month period, nothing works quite the way anyone would expect it to.
Eme remains in the PICU on drips and multiple electrolytes – some running continuously and others as needed. The goal now is to get her “good enough”. Good enough to go home. It won’t be perfect; it never has been & it never will be. Indeed good enough is just that; I’m hoping and praying it comes soon.
In honor of Emerson, I have a request – go outside and do something fun today… even if only for 5 minutes. Pause, then, and really appreciate the moment. Maybe if hundreds of people can genuinely imprint a summer memory today, it will somehow make up for the fact that we cannot. Summer is in full swing & we are painfully aware of all we’re missing in the world outside these glass walls.
Thanks, as always, for your support. We love you all 🙂
