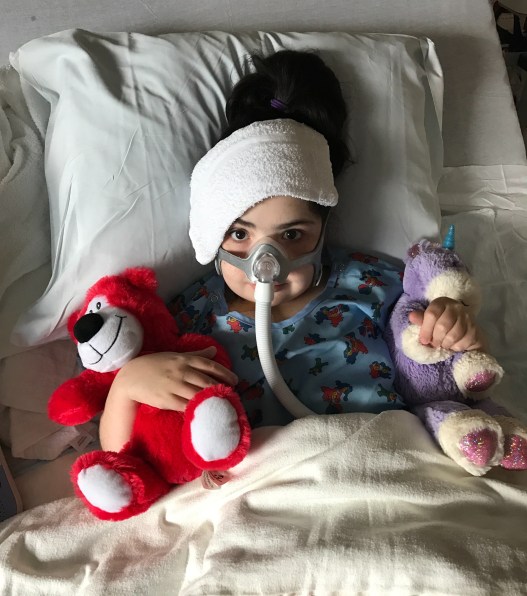
We’ve officially hit “that point” in this admission – I’m tired, cranky, frustrated, and ready to go. We know what’s wrong with Eme – we know what we can treat and we know what we cannot. We also know how she gets sick and we know how she recovers. Yes, she throws curveballs, but given that most all her organ systems are involved & affected by something, they’re usually in the context of a preexisting diagnosis. Her little body can’t handle too many new ones anymore.
Emerson is having trouble with her kidneys. It’s not a new phenomenon, but rather an exasperation of her usual presentation when sick. There are new minds involved this time, though, and with them have come new theories. And with new theories have come new treatment ideas. It’s all very encouraging. When it comes to things we’ve seen and managed before, I suppose it takes a heightened crisis for everyone to re-group and think outside the box.
Of course nothing comes without a few hiccups, but all in all Eme’s kidneys are slowly starting to recover. She continues to require frequent labs and electrolyte replacements, but urine output is finally trending down and we’re heading in the right direction.
Emerson’s skin is bruised and swollen from her brush with DIC and she’s still tired and very weak. Her kidneys have not yet recovered and she still has a few drips to wean off. We’ve talked to everyone, though, and they’ve agreed to let her discharge from the PICU. As soon as she’s off BiPAP & PICU meds, we should be able to go. If I had to guess, I’d say maybe (hopefully) next week.
I’m trying hard to be polite and political, to advocate with purpose and respect. I’ve hit “that point” though… I’m tired of being patient. I want to jump to the treatment most likely to work; I don’t want to prove 3 things won’t work first. I completely and logically understand why it’s best done that way, but I’m exhausted. Physically and mentally drained. And now that the adrenaline of this admission is starting to subside, my thoughts turn to the to-do list at home.
I’m not sure how many more gram-negative sepsis events my sweet girl has in her, but it seems at least one more. Thank you so much for your support over the past few weeks. Your comments and prayers were read and heard… each one meant more than you’ll ever know.
I’ll continue to update, but can safely say Eme is now “out of the woods” on this one 🙂